Non-infectious uveitis
Causes & symptoms
In particular with chronic uveitis (that persists for at least 3 months) that is not triggered by infections, noticeable symptoms don't tend to appear until late in the progression of the disease. They are usually discovered by chance during routine examinations. If any symptoms do appear, they are usually in the form a marked deterioration of the eyesight: many of those affected report blurred or unfocused vision; they also see streaks or black, flake-like spots that can appear in a fixed location or move around. Pain, markedly red eyes, excessive tear production and sensitivity to light may also occur as a result of uveitis. Uveitis may recur in episodes – if that happens, phases with symptoms and phases without symptoms tend to alternate.
Healthy eye
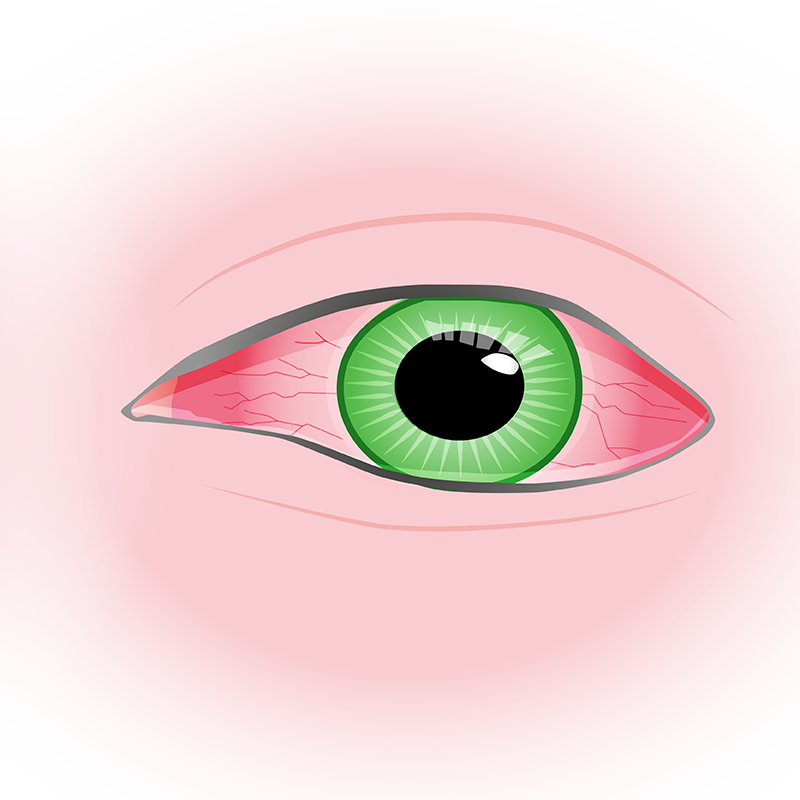
Uveitis
What causes non-infectious uveitis?
Up to now, no clear cause of the disease has been determined; however, researchers assume that non-infectious uveitis is an autoimmune disease. It may occur on its own or be the result of another underlying disease, e.g. rheumatic diseases such as axial spondyloarthritis and juvenile idiopathic arthritis, or chronic inflammatory bowel diseases, such as Crohn's disease and ulcerative colitis. Age and gender do not seem to play any role in the risk of developing uveitis. However, many of those affected display a certain genetic trait, medically known as HLA-B27.
It is important that uveitis and any underlying diseases that may be present are treated as early as possible, because, left untreated, the sight may then deteriorate until blindness occurs. Possible secondary diseases of uveitis are glaucoma and cataracts, clouding of the vitreous body, detachment of and fluid deposits in the retina as well as damage to the optic nerve.
